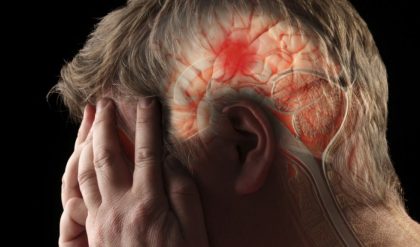
Traumatic brain injury, any damage to the brain from an applied force. The forces involved can be from direct contact, as in a blunt or penetrating head injury; from a gravitational source such as fierce shaking; or from rotational energy that produces shear stress between the brain and the skull. Often, a combination of forces is involved; for example, a motor vehicle collision can cause both direct blunt trauma and injury from rotational and rapid velocity changes. Those events cause a deformation of the brain tissue that results in several types of pathology. In addition to the primary injury (caused at the moment the force is applied), a series of events are set in motion that continue to cause cellular damage over the next days to weeks or even longer. Those secondary injury events include a complex set of biochemical reactions and molecular changes that extend cellular damage, brain edema (swelling), and inflammation in a self-perpetuating cycle that rapidly increases the extent of the brain damage.
Traumatic brain injury is broadly defined in terms of three categories of severity—mild, moderate, and severe—based on the Glasgow Coma Scale (GCS). The GCS is a 15-point scale designed to measure the patient’s ability to respond to visual, verbal, and motor stimuli after traumatic brain injury. The degree of impairment depends on the extent of damage to critical brain areas. The majority of traumatic brain injuries are mild. Nonetheless, traumatic brain injury is a significant cause of death. In the United States, for example, 40 percent of deaths from acute injury are due to traumatic brain injury. Traumatic brain injury is also a major source of disability, resulting in sometimes permanent impairment of physical and cognitive function.
Primary Injury
Direct contact with the skull or brain is classified as blunt trauma (e.g., from impact with a baseball bat or a windshield) or penetrating trauma (e.g., from gunshot wounds, shrapnel, or knives). Blunt contact causes injury directly below the contact point. The impact can also cause the brain to move or to shift back and forth inside the skull, damaging the opposite side of the brain, in a contrecoup injury. The base of the skull is bony and rough and can cause tearing and bruising to brain tissue when it bounces back and forth. The extent of damage varies with the intensity of force applied. The primary injuries that result are contusions (bruising of the brain tissue), tearing of the tissue and blood vessels, bleeding, tissue shearing, and disruption of neuronal networks. Blunt head injury may be closed or open, if the skull has been compromised to the point that brain tissue is exposed to the environment.
In addition to the direct blow, blunt trauma to the head causes the transmission of forces throughout the brain tissue. If strong enough, they can cause shearing and disruption of tissue and neural networks deep within the brain. That type of damage tends to be diffuse and can result in axonal damage (diffuse axonal injury, or DAI), diffuse edema, and extensive neuronal death. The damage can extend the secondary injury throughout the brain, to areas far from the point of original contact. The same acceleration forces that cause DAI can also cause stretching and tearing of blood vessels, leading to subcortical hemorrhages, additional neuronal damage, and disrupted functional activity in otherwise intact neurons.
Penetrating injury results in different injury patterns from blunt injury. The biggest factors in the degree of damage from a penetrating injury are the velocity and mass of the projectile. Shells from high-powered rifles and other high-velocity projectiles can cause an enormous pressure wave that damages the brain tissue in predictable patterns and can be massive and devastating. Lower-velocity projectiles cause less pressure-wave damage and less direct shrapnel path damage. As with blunt traumatic brain injury, penetrating injury sets off a secondary injury cascade.